The analysis below reflects our thoughts on the Direct Contracting Model at the time of its inception in 2020. The model has since evolved into ACO REACH. Read our most up-to-date analyses on the new model, and how to succeed.
Earlier this year, the Center for Medicare and Medicaid (CMS) announced five new payment models designed to transform primary care by paying providers for outcomes rather than services.
Direct Contracting and Primary Care First are two of these models announced by CMS to help encourage providers and other eligible professionals to shift from FFS to value-based payments. HHS Secretary Alex Azar calls the new payment models “the biggest step ever taken toward” value-based payments in primary care.1 Azar states the models will test out paying for health and outcomes rather than procedures on a much larger scale and is designed to encourage state Medicaid programs and commercial payers to adopt similar approaches.1
Although these models are considered voluntary and therefore experimental, this is not the first and most certainly not the last we’ve seen of these core concepts. These primary care models build on some of the recent changes to Medicare Shared Savings Program (MSSP) and the new “Pathways to Success” program.
While the “Pathways to Success” program is focused on specific groups in a risk-sharing arrangement, Direct Contracting is CMS’s attempt at re-engaging those providers and organizations who are no longer in the MSSP Program as well as expanding the reach to allow other providers to take on downside risk.
How ACO REACH Compares to Direct Contracting
What is Direct Contracting?
Direct Contracting is a voluntary, five-year (plus an optional implementation year) alternative payment model (APM) which leverages components from the Next Generation ACO Model (NGACO), Medicare Advantage (MA), and the private sector and will be the focus of today’s write-up.
DC’s goals are to:
- Transform risk-sharing arrangements in Medicare Fee-For-Service (FFS)
- Empower beneficiaries to personally engage in their own care delivery
- Reduce provider burden to meet health care needs effectively
Direct Contracting Entities (DCE) form relationships with two types of providers and/or suppliers: Participant and Preferred Providers. There are two key differences between these relationships. First, beneficiaries can only align to Participant Providers, not Preferred Providers. Secondly, Participant Providers are required to enter a negotiated payment arrangement with the DCE, while Preferred Providers can elect to receive this negotiated payment or not. Direct Contracting Entities should consider these differences when deciding what relationship to form with which providers.
Direct Contracting contains three types of risk arrangements, only two of which are available to participants today. These arrangements are intended to encourage organizations to take on more downside risk. The two risk options, professional and global, are a 50% and 100% shared savings/losses arrangement, respectively.
There are three DCE Types, Standard, New Entrant, and High Needs, each of which is eligible with the various risk arrangements. The Standard DCE Type is for DCEs with substantial historical claims-based experience serving Medicare FFS. This type is for any NGACO organization looking to transition to the DC payment model and projected to be a majority of the applicants. The New Entrant Type are for DCEs with limited experience delivering care to FFS beneficiaries whereas the High Needs Type are for DCEs that focus on beneficiaries with complex, high needs, including individuals with dually eligible for Medicare and Medicaid, similar to the Seriously Ill Population for the Primary Care First.
The key dates around Direct Contracting Activities can be found below.
| Activity2 | Date2 |
|---|---|
| Letter of Intent | December 12, 2019 |
| Application for PY1 Due | July 6, 2020 |
| Performance Year 0 Begins (Implementation Period) | October 1, 2020 |
| Performance Year 1 Begins | April 1, 2021 |
| Performance Period Ends | December 31, 2025 |
Why Understanding Risk Scoring in the ACO REACH Model is Critical For Success
One major concern about the Direct Contracting model was risk scoring abuse. Read how the updated model plans to address risk scoring.
Why DC?
CMS believes that DCEs having control of funds with their downstream providers will enable them to improve care coordination and delivery and to better manage the health needs of their aligned beneficiary population, resulting in reduced costs and better outcomes. As such, the proposed payment mechanism will be paid out monthly directly to the DCE. The hope is that the DCE will invest in technology, expand resources necessary for value-based care (VBC), and reimburse providers through payment arrangements. As part of the payment mechanisms, DCEs can select Advanced Payments in addition to Capitation Payment Mechanisms. DCEs have the option to select either Primary or Total Care Capitation. The Primary Care Capitation (PCC) option is available for both Global and Professional Risk Arrangements and is a capitation model for defined primary care services. The Total Care Capitation (TCC) option is only available for the Global Risk Arrangement and is a capitation model for the total cost of care. DCEs receive a monthly capitated payment from CMS in lieu of their providers FFS claims thereby encouraging providers to keep total cost of care down. More details can be found here.3 For more information, please reach out to your CareJourney representative.
Benchmarks vary on the DCE type chosen and beneficiary alignment type. The benchmark is a Per Beneficiary Per Month (PMPM) dollar amount which is used to hold DCEs accountable for FFS expenditures for their beneficiaries. The benchmark consists of Part A and B total cost of care and are calculated separately for the Aged & Disabled and ESRD cohorts. CMS will use the following benchmark calculation process to determine shared savings or losses due for each DCE4:
- Calculate Historical Expenditures
- Trend Baseline with USPCC
- Apply Risk and Geographic Standardization
- Incorporate Regional Expenditures (MA Rate Book)
- Adjust for Risk and Geography for Performance Year
- Apply Discount / Quality Withhold
It’s important to be able to calculate the historical expenditures, which the CareJourney analysis will allow you to do. The historical baseline expenditure is calculated using a weighted average of historical Medicare expenditures for beneficiaries that would have been aligned to the DCE in the base years (2017-2019).4 It should be noted that although the base years will always remain constant, the historical baseline expenditures will change for each performance year as CMS will use the most recent list of Participant Providers.3
| Baseline Year | 2017 | 2018 | 2019 |
|---|---|---|---|
| % Contribution to Historical Baseline | 10% | 30% | 60% |
For beneficiaries voluntarily aligned, historical expenditures will begin in PY4 where they will use a modified weighting.
| Baseline Year | 2021 | 2022 | 2023 |
|---|---|---|---|
| % Contribution to Historical Baseline | 33% | 10% | 67% | 30% | 60% |
What Are We Hearing From Members?
After speaking with our members, it’s clear several are interested in better understanding the payment model and whether it’s the right decision for them. Although not all of our members are planning to participate in Direct Contracting, a large number are. Others are interested in participating in Primary Care First and others will be staying in the Medicare Shared Savings Program. Below is a list of the payment models that CMS has released with a particular focus on primary care in an effort to improve health and reduce costs by redesigning primary care.5
| Level of Risk5 | Payment Models5 |
|---|---|
| Low | Primary Care First |
| Medium | MSSP Enhanced Track |
| High | Direct Contracting |
Some of the common questions we are hearing from our member base is around projecting historical benchmark calculations, understanding beneficiary counts, and voluntary alignment opportunities.
Key Decision Points
There are a number of key decision points that will need to be made prior to the implementation and/or performance period. Several of the key decisions are listed below. The CareJourney Direct Contracting Analysis will provide the key analytics needed to make an informed decision. Should you have any additional questions regarding each of the decision points below, please feel free to reach out to your CareJourney representative.
- Do I have a current or legacy TIN that I want to participate with? Or do I need to form a new one?
- Do I meet the minimum level for the number of beneficiaries for the program?
- Do I need to worry about another Shared Savings program?
- Who do I add to my Participant Provider to the Provider list?
- Should I add specialists to my Participant Provider to the Provider list?
- Who do I add to my Preferred Providers to the Provider list?
- Does my entity have any providers that are billing under multiple organization billing NPIs, that could potentially be under another TIN, that I have to be worried about?
Common Approaches to the Implementation Period
The implementation period is intended to help New Entrants DCEs build an aligned FFS population by testing enhanced opportunities for voluntary alignment. This period provides DCEs with additional time to engage in alignment activities and plan their care coordination with management strategies prior to the first performance year.6
After speaking to our member base, we are seeing a few different approaches to the implementation period which is found below.
Option A: Select an Existing TIN and test Voluntary Alignment Activities
Option B: Select an Existing TIN and test DCE Leakage Shifts
Option C: Select a Handful of Providers (new TIN) and test Voluntary Alignment Activities
Option D: Select a Handful of Providers (new TIN) and test DCE Leakage Shifts
After speaking to the organizations that use an existing TIN, they plan on entering the performance period with the entire TIN or are planning to form a new TIN depending on their progress under the implementation period. For their providers with high leakage and a high total cost of care, they’re particularly focused on improving both of those metrics to be included in the new TIN. Unfortunately, there is no one-size-fits-all approach but each of the above options have their pros and cons and it is up to the DCE to determine what approach works best for them.
- Voluntary Enrollment efforts
- Leakage
- Total Cost of Care
- Types of DC
- Participant/Preferred Providers
For organizations looking for more guidance on Direct Contracting, NAACOS has launched a direct contracting taskforce7 and America’s Physician Group’s Risk Evolution Task Force is also focused on helping organizations take on Direct Contracting.
Explore with CareJourney
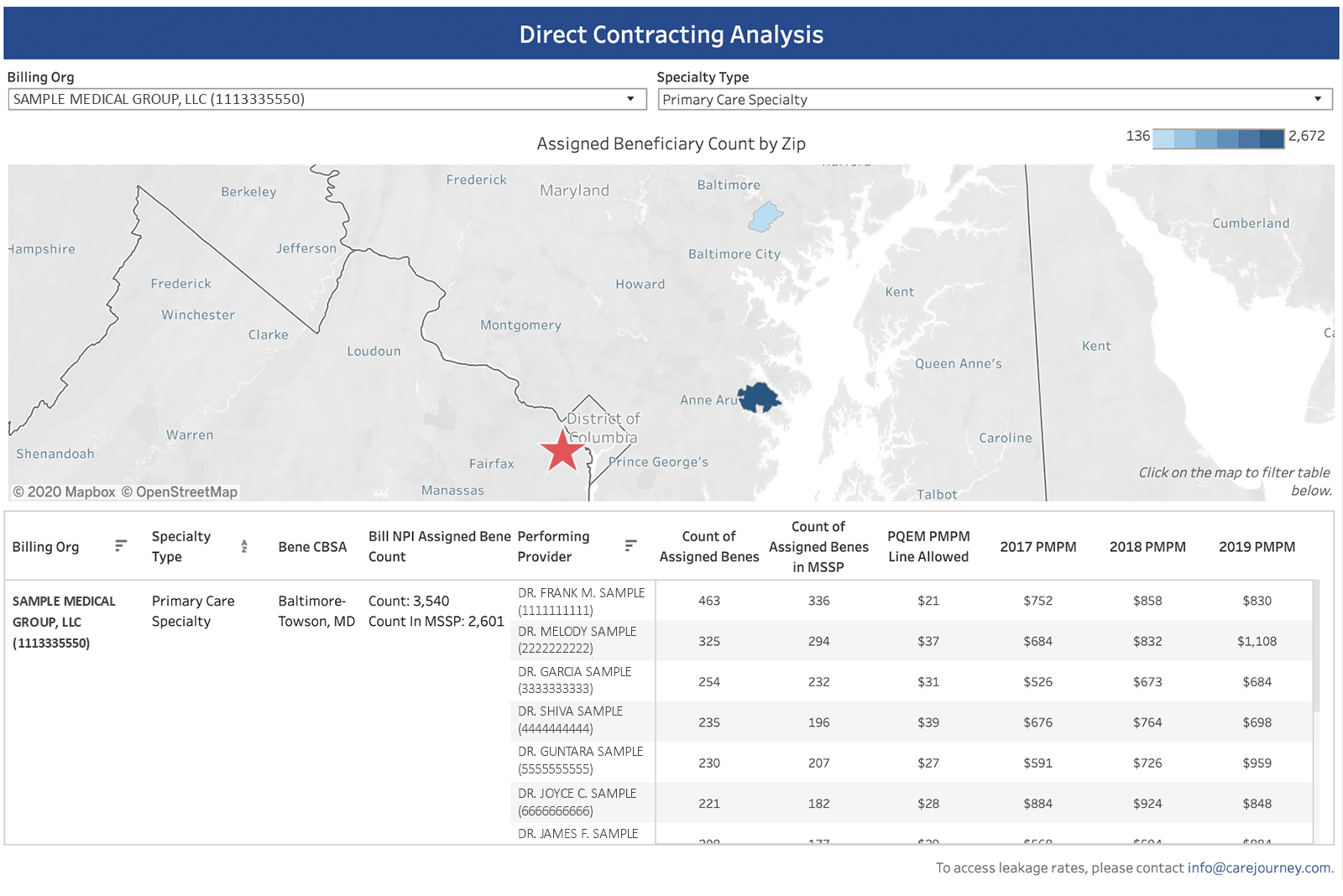
Want to understand the historical performance of your Provider Participants to better project how they will perform under DC?
CareJourney has the tools necessary to help you make the best decision for both the implementation and performance periods. From providing historical performance details, to projecting your claims assigned beneficiaries, to measuring performance during the implementation/performance periods, to helping you set up Data at the Point of Care or Blue Button.
- Advisory.com. (2020). HHS just unveiled 5 new value-based payment models. [online] Available at: https://www.advisory.com/daily-briefing/2019/04/23/primary-care-model?WT.ac=Inline_A LL_DBA_x_x_x_PN_2019May22_Eloqua-RMKTG+Blog
- Innovation.cms.gov. (2020). Office Hours: Direct Contracting Model Options – Benefit Enhancements and Application Overview | Center for Medicare & Medicaid Innovation. [online] Available at: https://innovation.cms.gov/resources/dc-model-options-benefit-app-overview.html
- Innovation.cms.gov. (2020). Direct Contracting: Global and Professional Options Payment Part One Webinar | Center for Medicare & Medicaid Innovation. [online] Available at: https://innovation.cms.gov/Files/slides/dc-model-options-paymentone-slides.pdf
- Innovation.cms.gov. (2020). Direct Contracting: Global and Professional Options Payment Part Two Webinar | Center for Medicare & Medicaid Innovation. [online] Available at: https://innovation.cms.gov/Files/slides/dc-model-options-paymenttwo-slides.pdf
- Innovation.cms.gov. (2020). Primary Cares Initiative Overview of Direct Contracting: Global PBP and Professional PBP Options | Center for Medicare & Medicaid Innovation. [online] Available at: https://innovation.cms.gov/Files/slides/dc-model-options-overview-slides.pdf
- Innovation.cms.gov. (2020). Direct Contracting (Professional and Global) Frequently Asked Questions | Center for Medicare & Medicaid Innovation. [online] Available at: https://innovation.cms.gov/Files/x/dc-faqs.pdf
- Modern Healthcare. (2020). NAACOS launches new direct contracting taskforce. [online] Available at: https://www.modernhealthcare.com/accountable-care/naacos-launches-new-direct-contracting-taskforce
