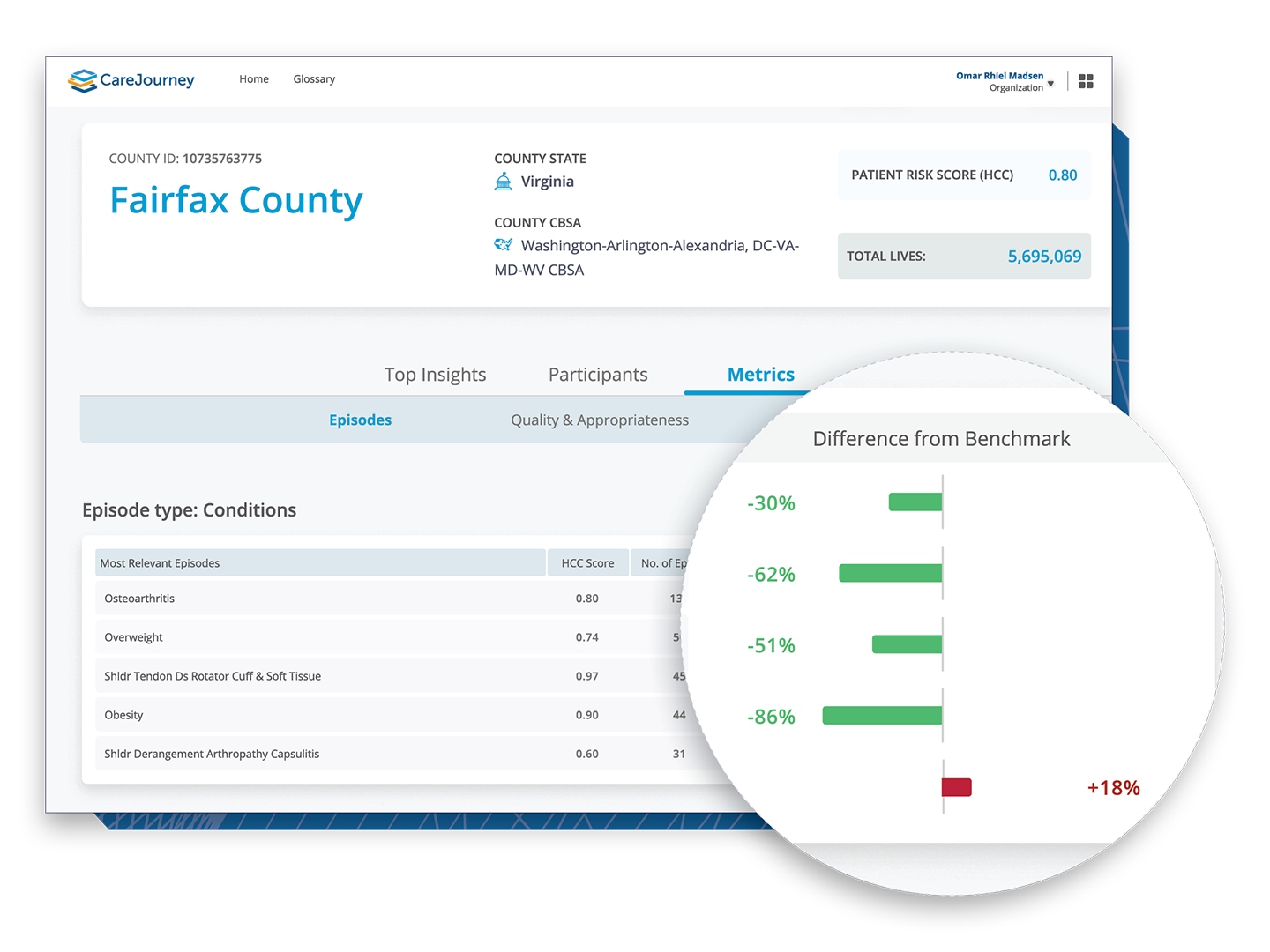
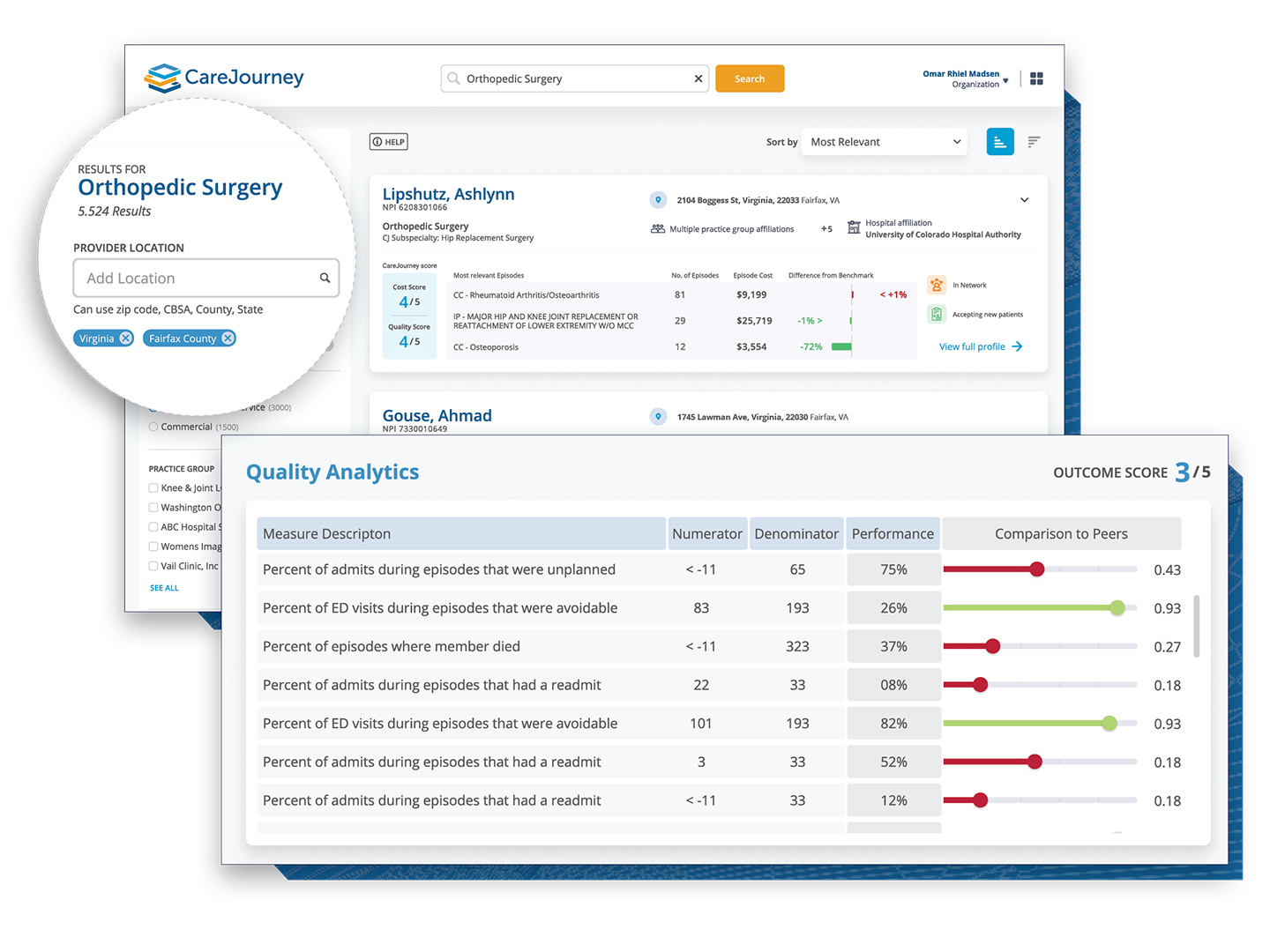
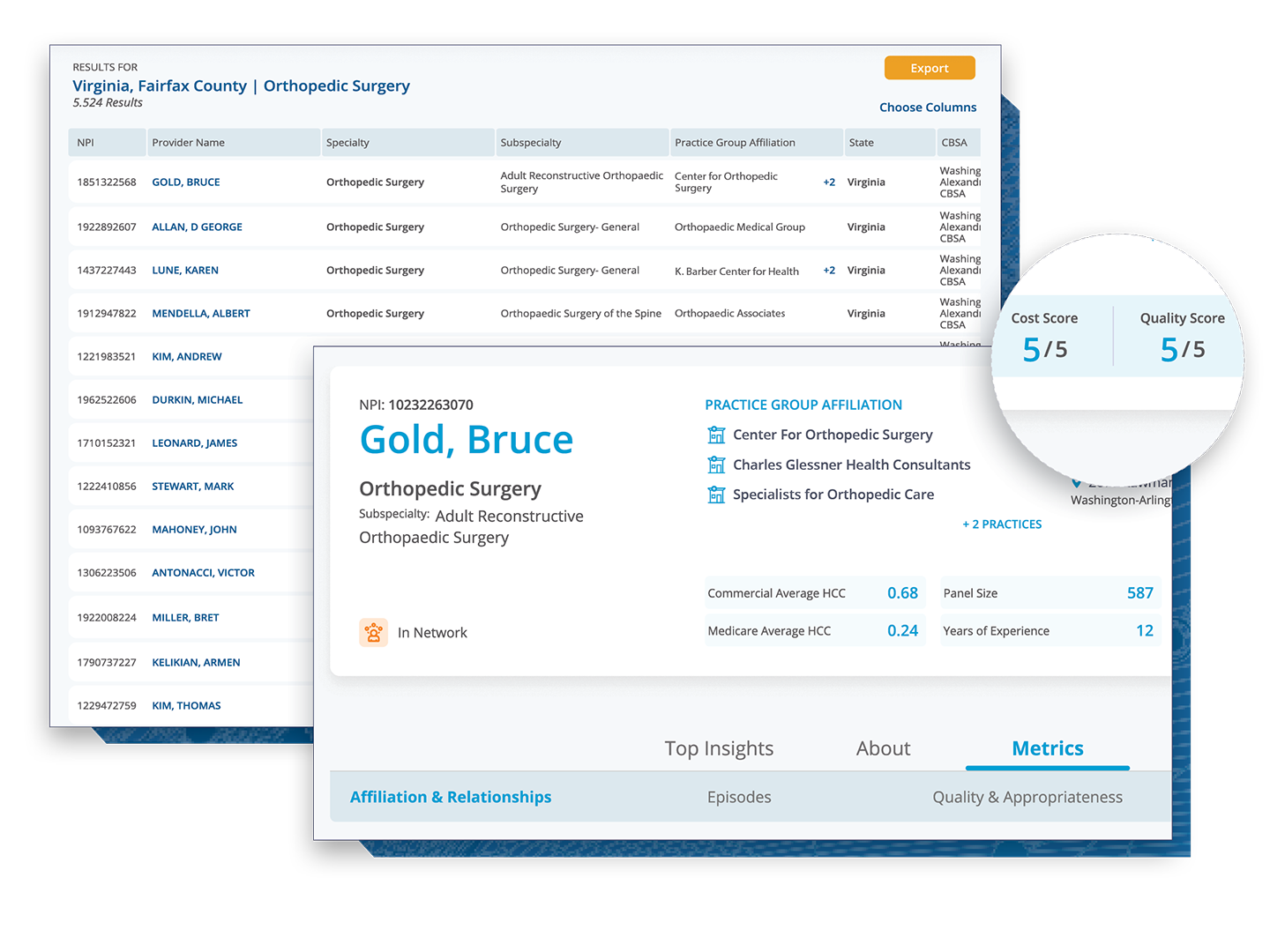
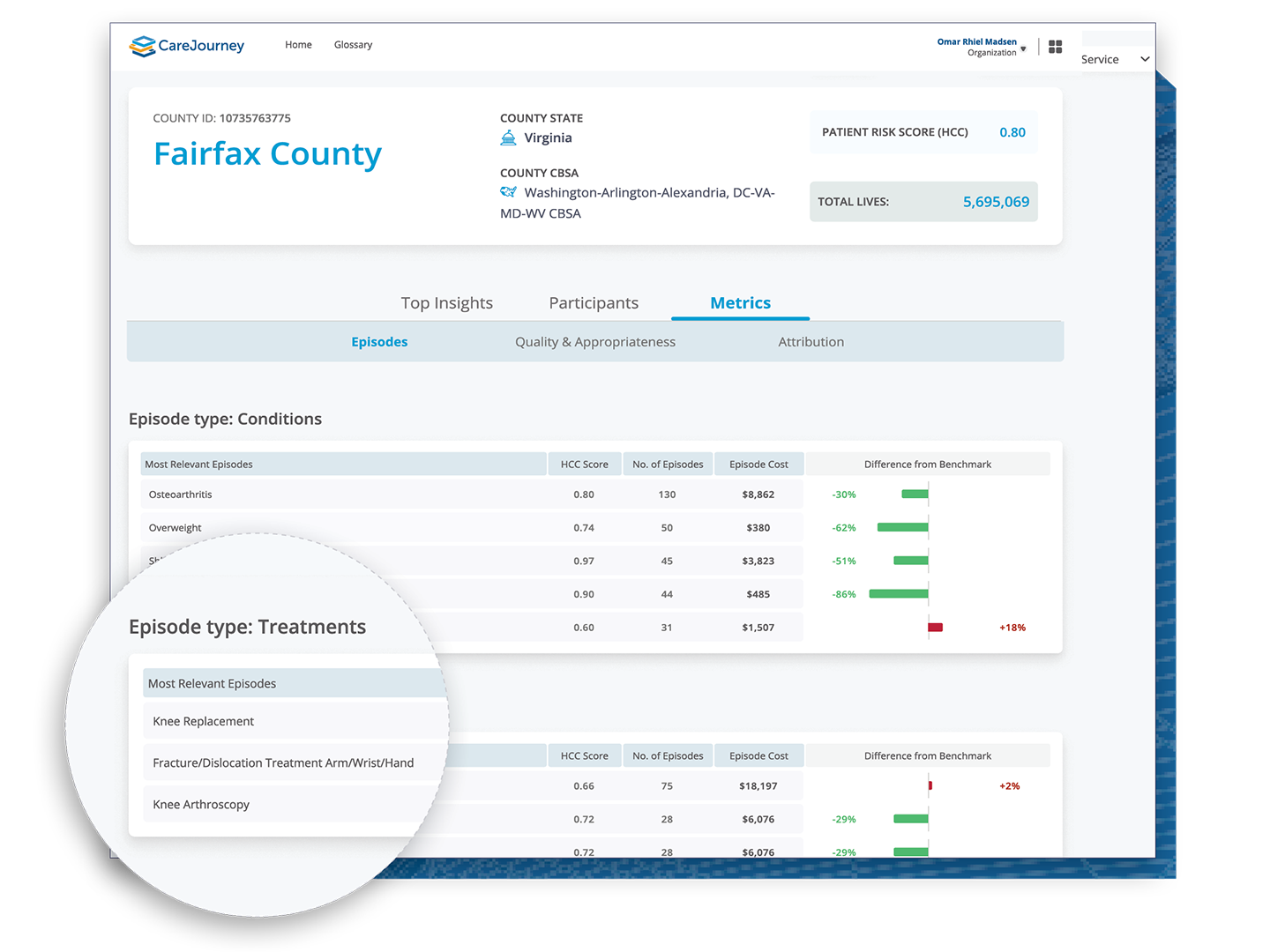
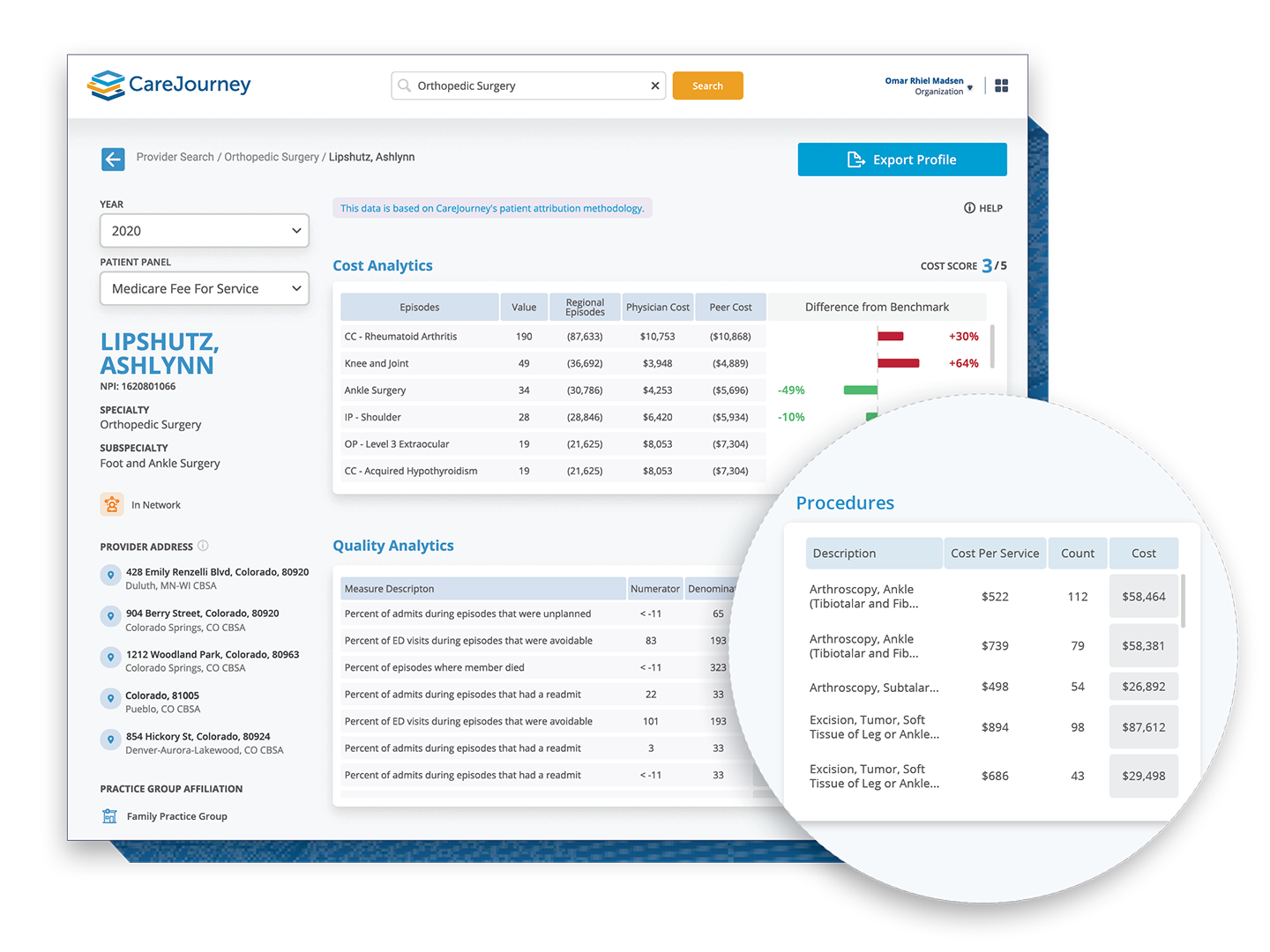
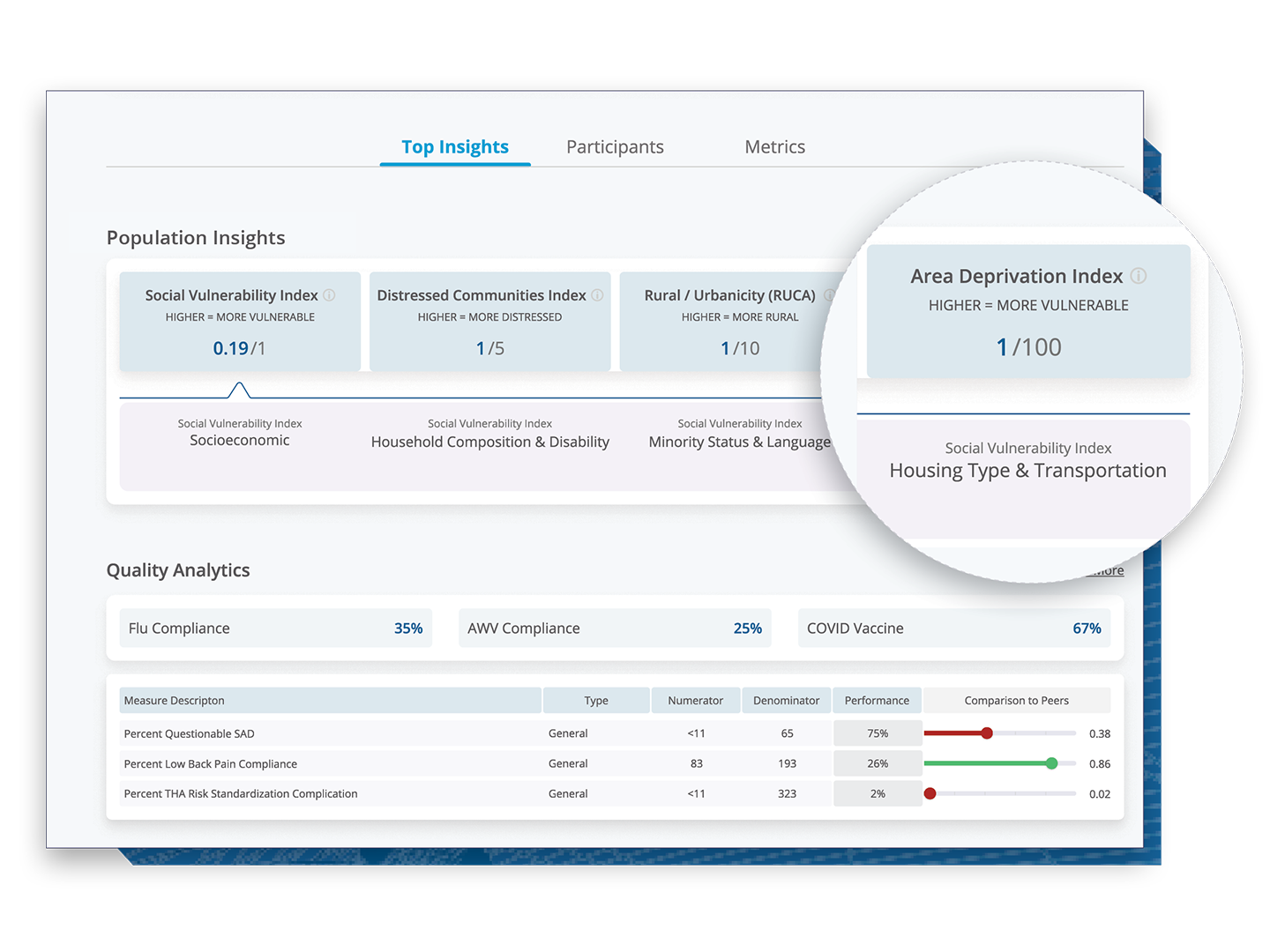
Analytics Driven by the Most Comprehensive, Longitudinal Data Set Available
0M+
Lives Covered
0M+
Providers Profiled
0+
Episodes Benchmarked
Expand Your Value-based Care Knowledge with Help From the Experts
The Smartest Minds in Health Care Trust CareJourney Analytics