For Provider Organizations That Want to
Excel in Value-based Care
With the shift from fee-for-service reimbursements to value-based care, providers are assuming more financial risk than ever. This means you are balancing your ability to provide the best care while ensuring profitable network growth, and managing the complexities of new payment models.
Our healthcare provider analytics help you make more informed decisions around network development/expansion, performance improvement, referrals management, care variation, coordination, and quality. Our access to comprehensive Medicare, Medicaid, and Commercial datasets – linked claims and encounter data for over 300 million longitudinal beneficiaries – powers our healthcare provider analytics and solutions, designed specifically for you.

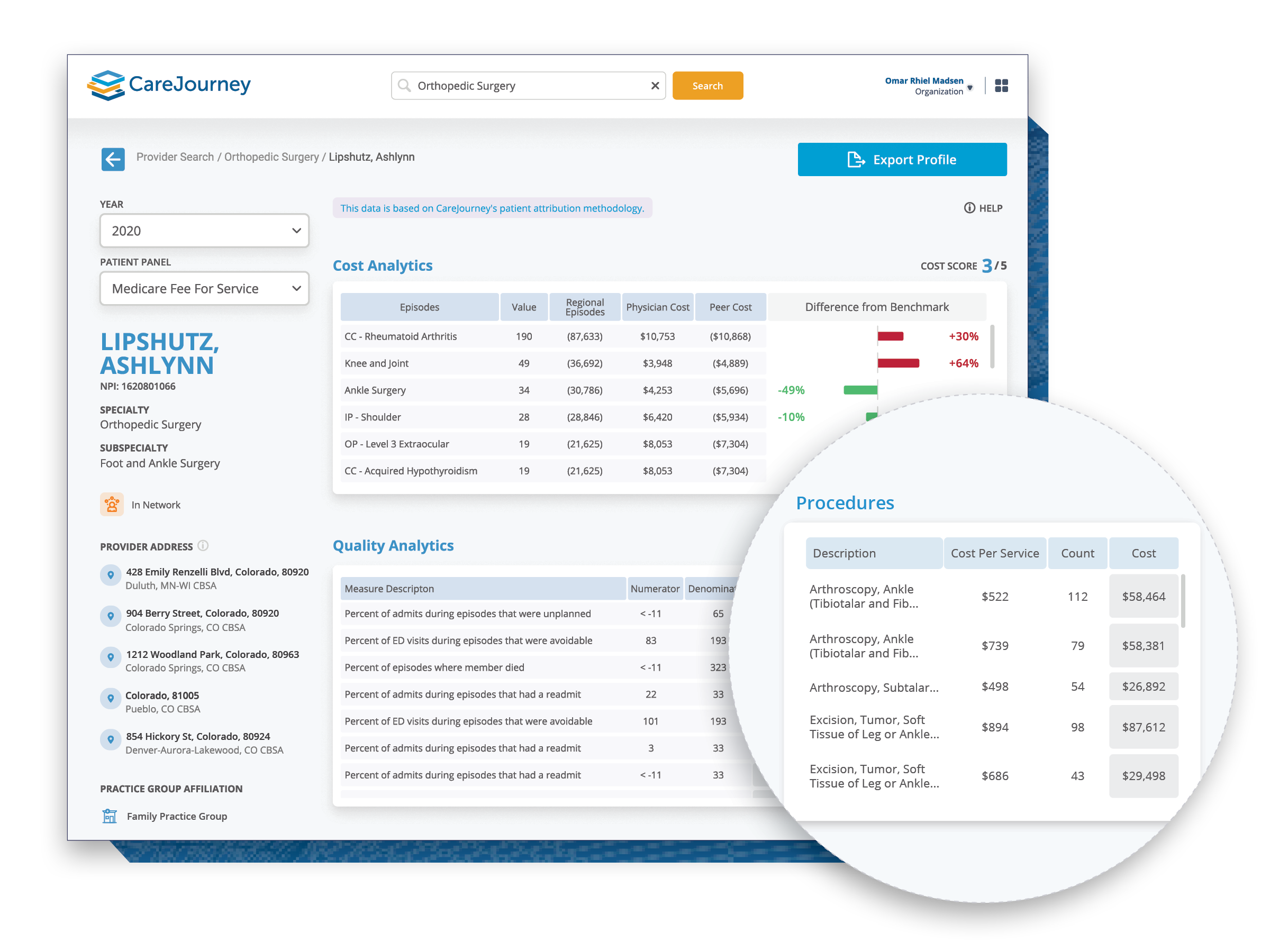
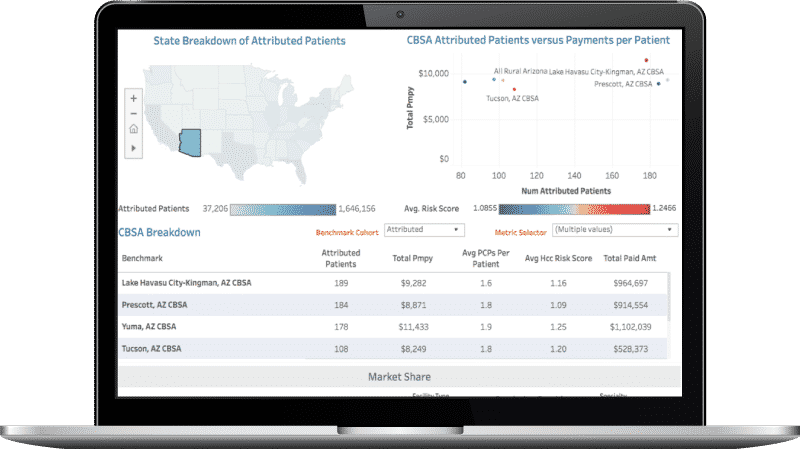
Our analytics platform offers clinically-relevant insights to understand market share, identify high-need patients, build high-performing networks, and improve provider performance and patient outcomes. It is powered by one of the largest claims datasets in the country that is backed by comprehensive and transparent methodologies.
Find all the relevant information needed to be successful in value-based care, all in one place.


“Amazing as a clinician and ACO leader to have a hunch about common medical problems! It helped us uncover a great opportunity for a win. We reduced avoidable UTI admissions, hospital spending and patient suffering, the whole triple aim!”
Dr. Joshua Lowentritt, MD
Chief Medical Officer
Louisiana Physicians ACO
Identify facility specific volumes and costs by episode of care.
Identifying high performing providers to include in referral network for specialty care.
Implementing a high-need, high-cost patient segmentation model to decrease the total cost of care.