Background
According to the American Heart Association, more than 1.5 million people in the United States experience a heart attack or stroke each year, with heart disease and stroke consistently among the top causes of death and disability. This costs the US healthcare system over $350 billion annually.1 However, heart attacks and strokes are, in many cases, preventable.
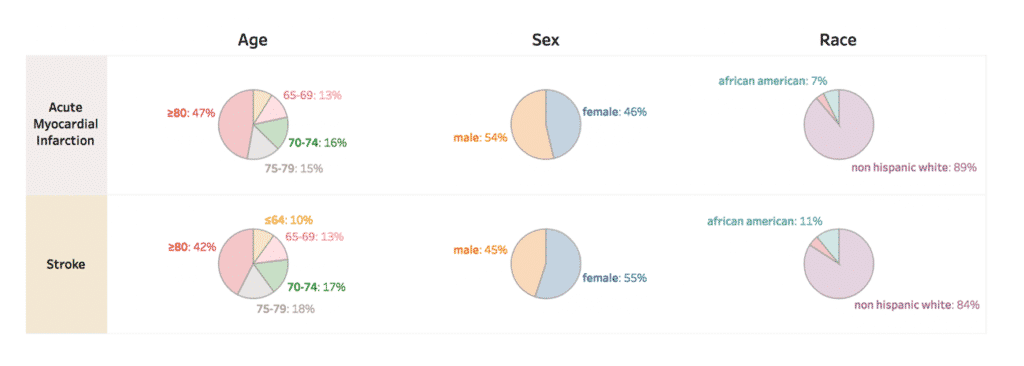
Source: CareJourney’s Cohort Atlas platform
In the midst of the COVID-19 crisis, hospitals have seen drastic reductions in admissions for heart attacks and strokes; in an informal poll, well over half of cardiologists reported reductions in admissions for heart attacks of 40 percent or more.2
Providers worry that this pattern is not due to a true reduction in cases – times of disruption and stress would likely mean more cardiovascular events – but likely, a desire among the general public to avoid seeking treatment for fear of catching the virus, until the situation becomes dire.
This striking trend underscores the importance of prevention, early intervention, and public education around cardiovascular risk factors and disease.
The Million Hearts Initiative
Million Hearts is a national initiative aimed at improving cardiovascular health for all Americans. The goal of Million Hearts is to reduce heart attacks, strokes, and other cardiovascular events by one million every five years.3 Originally launched in 2012 and jointly led by CMS and the CDC, Million Hearts outlines specific tactics for states and healthcare providers, focusing on a small set of priorities that have been proven to have a significant positive impact on heart health and disease reduction, including:
- Keeping people healthy through positive environmental and behavioral changes
- Optimizing care to get patients with cardiovascular risk the services they need
- Improving outcomes for priority populations who are at higher risk for cardiovascular disease4
Leveraging CareJourney’s access to the all Medicare fee-for-service claims database, we are able to gain insight and a benchmark for the latter two priorities of Million Hearts, mentioned above.
Million Hearts Population Explorer: An Interactive Dashboard
Explore heart attack and stroke rates, as well as cardiovascular-related chronic condition prevalence, for priority demographic populations for care optimization and early intervention.
Million Hearts Cardiovascular Disease Risk Reduction Model
To better understand the efficacy of the Million Hearts Model, CMS developed the Million Hearts Cardiovascular Disease Risk Reduction Model, a randomized controlled trial focused on Medicare beneficiaries. Launched in 2017, the five-year evaluation aims to inform decision-making about scaling the model by assessing if and how Million Hearts interventions improve cardiovascular disease care, reduce heart attacks and strokes, and reduce spending.5
516 organizations were divided between an intervention group, who were tasked with implementing the ASCVD risk calculator (detailed below) and other evidence-based interventions, and a control group, who did not change their practices but submitted data to CMS for comparison. Initial findings suggest favorable effects of the Million Hearts model on the delivery of CVD preventive care and prescription adjustment, reduction of risk scores among high-risk patients, and fatality reductions among medium and high risk beneficiaries.6
ASCVD 10-Year Risk Calculator & Impact of Comorbidities
A tool heavily employed in Million Hearts efforts, the Atheroscledrotic Cardiovascular Disease (ASCVD) 10-Year Risk Calculator estimates a patient’s risk of having a cardiovascular event within 10 years, based on demographic data and patient health history. The American College of Cardiology and the American Heart Association encourage providers to use the tool with patients to develop prevention and treatment plans.
The ASCVD calculator takes into account several comorbidity indicators, including history of diabetes, hypertension treatment status, and tobacco use history, to predict patient cardiovascular risk. Leveraging claims data, we are able to clearly see the compounding effects of these and other cardiovascular-related comorbidities on history of heart attack and stroke, as shown in the charts below.
Heart Attack & Stroke Prevalence by Comorbidity Count, All Beneficiaries, 2019
Comorbidities considered: CHF, Hypertension, Ischemic Heart Disease, Diabetes, Asthma
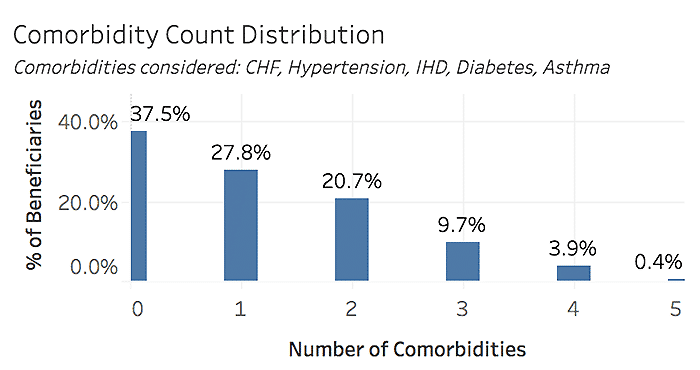
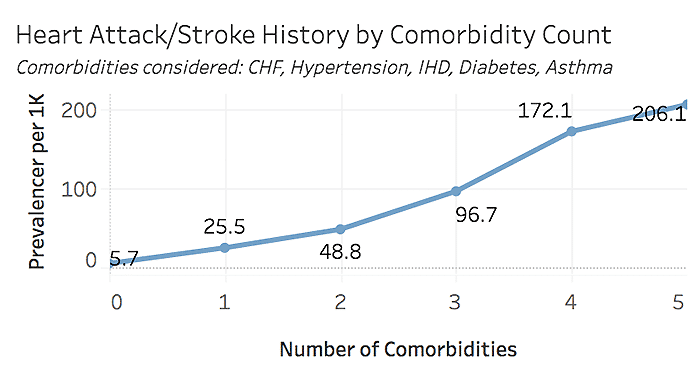
Heart Attack & Stroke Prevalence by Comorbidity Count, Beneficiaries with Tobacco Use, 2019
Comorbidities considered: CHF, Hypertension, Ischemic Heart Disease, Diabetes, Asthma
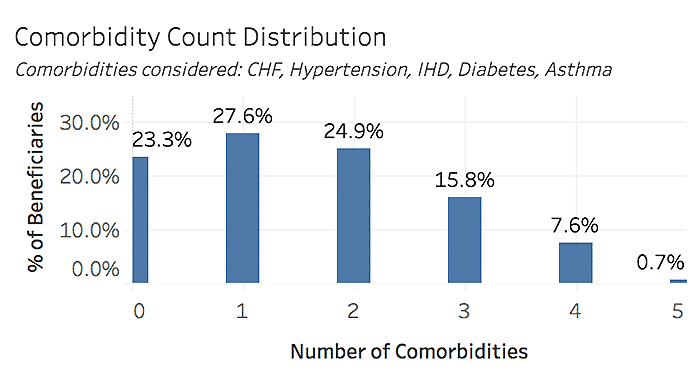
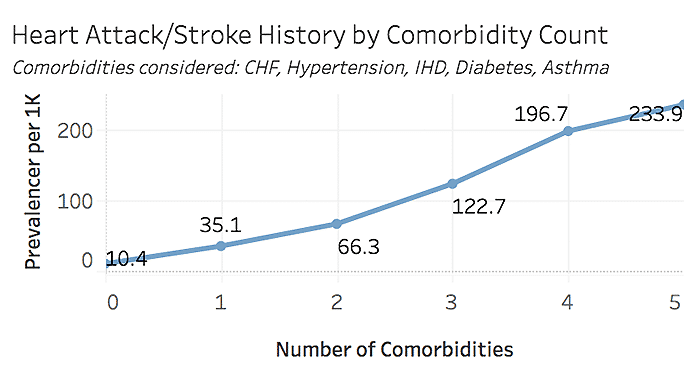
Note: Data focus on target population for the Million Hearts Cardiovascular Disease Risk Reduction Model, which includes Medicare fee-for-service patients ages 40-79, and excludes those in hospice or who have end-stage renal disease (ESRD).
As shown above, more than half of beneficiaries have at least one of the chronic conditions of focus, and more than 75% of tobacco users have at least one condition. While the rate of heart attack or stroke history is low among those with 0-1 chronic conditions, the incidence rate increases steadily with additional chronic risk factors. Of course, not all conditions carry the same risk; further detail on the history of heart attack or stroke prevalence by specific comorbidity combinations can be seen below.
History of Heart Attack or Stroke Prevalence Rates by Comorbidities, 2019
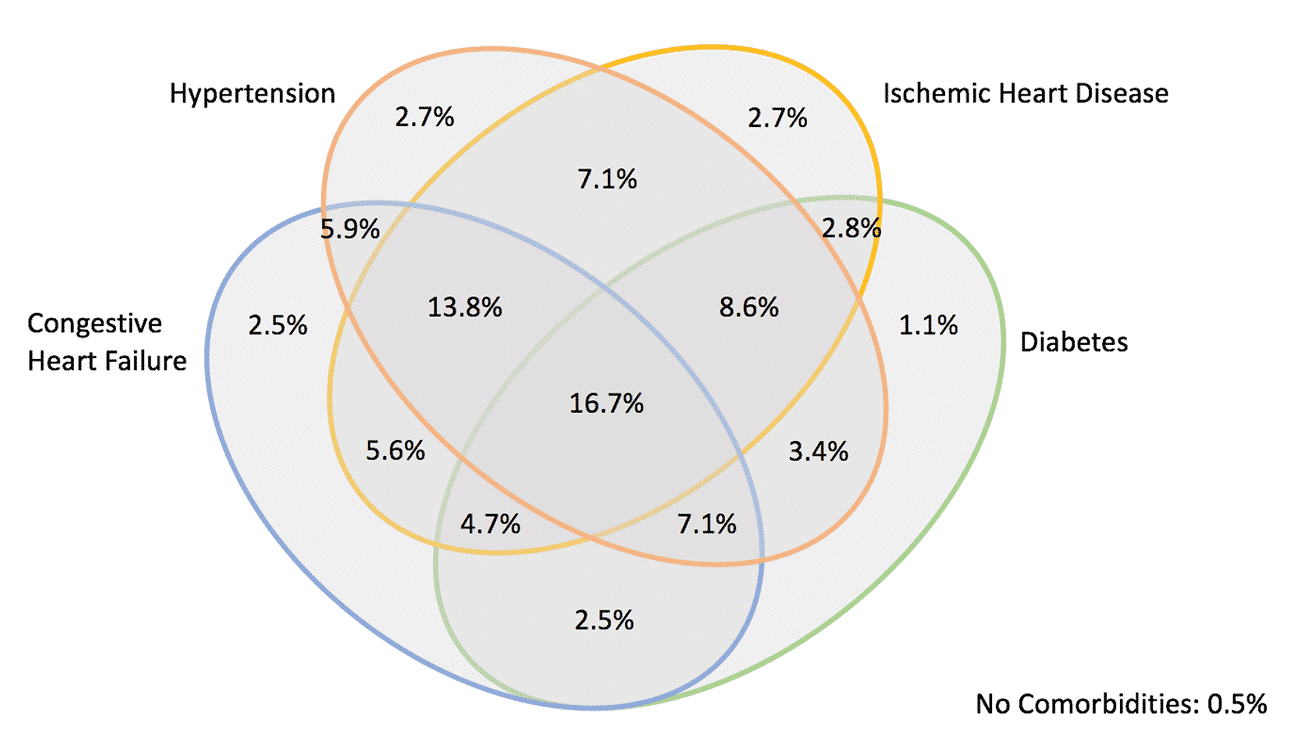
For instance, 13.8% of patients with a history of CHF, hypertension, and IHD have a history of heart attack or stroke; an additional diagnosis of diabetes increases this rate to 16.7%. Even a diagnosis of hypertension alone – something nearly half of beneficiaries have – yields a 2.2% prevalence increase compared to those without hypertension.
Bolstering the Million Hearts Approach through FHIR-Enablement at MedStar
Over the course of 2019, CareJourney’s Interoperability Advisory Services team supported the MedStar Institute for Innovation and the MedStar Health National Center for Human Factors in Healthcare in developing a FHIR-enabled app to integrate the ASCVD calculator into MedStar’s electronic health record system. This project was funded through a 2018 Leading Edge Acceleration Projects (LEAP) award through the U.S. Department of Health and Human Services (HHS) Office of the National Coordinator (ONC) for Health Information Technology. MedStar – one of two award winners of nearly $2 million in combined funding – set out to use FHIR standards to advance clinical knowledge at the point of care, and decided to do so through the lens of Million Hearts.
The integration of the ASCVD calculator into MedStar’s EHR significantly reduced the barrier to entry for using the tool, enabling the calculator to populate with patient demographics and health metrics directly from the EHR, rather than requiring a provider to type in all of a patient’s data into a separate platform. Officially launched in February 2020, the MedStar solution has two components: a clinician-facing estimation tool that enables providers to determine risk and develop treatment plans more easily in the clinical workflow, and a patient-facing education tool that empowers patients to understand the potential impacts of various interventions and lifestyle changes.7 Initially launched to 575 providers across 10 MedStar Health hospitals, ambulatory, and urgent care centers,8 the solution is now available to over 1000 providers.
The CareJourney team is excited by this important development and the opportunities it presents in furthering the mission of Million Hearts.
Explore with CareJourney
This exploration of the Million Hearts Initiative is just one example of the ways that CareJourney can leverage access to the Medicare fee-for-service all-claims database to codify leading care models, and illuminates some of the top-of-mind questions we explore with our members:
- What are the actionable cardiovascular patient sub-cohorts and what interventions exist to take better care of these patients?
- Which PCPs in your current or future network are treating a high number of patients at increased cardiovascular risk?
- Which healthcare providers and facilities are excelling at managing complex cardiovascular patient populations? What can we learn from them?
- What are quality and savings opportunity gaps that can help improve the cardiovascular and preventive care provided to these patients?
We look forward to working with your organization to improve cardiovascular care and population heart health. Please reach out to your Member Services representative for more information. If you’re not a CareJourney member, email us at jumpstart@carejourney.com, or you can learn more by requesting a meeting below.
- Benjamin, Emelia J., et al. (2019). Heart Disease and Stroke Statistics—2019 Update: A Report From the American Heart Association. Circulation, 139(10), e56–e528. Retrieved from https://www.ahajournals.org/doi/10.1161/CIR.0000000000000659
- Krumholz, H. M. (2020, April 6). Where Have All the Heart Attacks Gone? The New York Times. Retrieved from https://www-nytimes-com.cdn.ampproject.org/c/s/www.nytimes.com/2020/04/06/well/live/coronavirus-doctors-hospitals-emergency-care-heart-attack-stroke.amp.html
- CDC. (2018, September 6). Preventing 1 Million Heart Attacks and Strokes. Retrieved from https://www.cdc.gov/vitalsigns/million-hearts/index.html. Note that the goal of 1 million amounts to a 6% reduction in cardiovascular events.
- CDC. (2019, November 8). About Million Hearts®. Retrieved from https://millionhearts.hhs.gov/about-million-hearts/index.html
- CMS. (2020, April 22). Million Hearts®: Cardiovascular Disease Risk Reduction Model. Retrieved from https://innovation.cms.gov/innovation-models/million-hearts-cvdrrm
- Mathematica (2019, November). Evaluation of the Million Hearts® Cardiovascular Disease Risk Reduction Model: Second Annual Report. Retrieved from https://downloads.cms.gov/media/millionheartscdrrm-secondannualevaluationreport_1_13_20.pdf
- MedStar Institute for Innovation. (2020). Heart Risk Calculator. Retrieved from https://mi2.medstarhealth.org/about-us/featured-projects/heart-risk-calculator/?opt_id=oeu1580149449398r0.14210662507683347&_ga=2.5554291.1726096339.1582735146-1131135538.1580149450
- MedStar Health. (2020, February 26). MedStar Health Launches New Interactive Heart Risk Calculator in Patient Electronic Health Record. Retrieved from https://www.medstarhealth.org/mhs/2020/02/26/medstar-health-launches-new-interactive-heart-risk-calculator-in-patient-electronic-health-record/
