Update: While CareJourney was disappointed to hear that the Seriously Ill Population component is currently underway by CMS, we are extremely excited that the Primary Care First model has introduced an additional cohort to start in January 2022! Be sure you’re informed before entering the model and well equipped for success. Contact CareJourney for more information.
Background
Earlier this year, the Center for Medicare and Medicaid (CMS) announced five new payment models designed to transform primary care by paying providers for outcomes rather than services. One of the payment models is the Primary Care First (PCF) Model which is a voluntary, five-year alternative payment model (APM) aimed at reducing Medicare spending via prevention of acute hospital utilization, improving doctor-patient relationship, improving care for patients with complex chronic needs, and seriously ill patients.
The PCF model consists of two payment options in which eligible providers can choose to participate in either one or both. The first “General” (PCF-General) option introduces higher payment for primary care practices caring for complex, chronically ill patients and the second “High Need Population” also known as the “Seriously Ill Population” (PCF-SIP) option, encourages advanced primary care practices that typically provide hospice or palliative care services to take responsibility for a high-need population.
Eligible practices will have an opportunity to increase their revenue with geographically adjusted performance-based payments and will be focusing on a single outcome measure, acute care hospitalization. Practices also have the potential to become a Qualifying APM participant.
To participate in the PCF model, practices must be located in one of the 26 PCF regions, include Primary Care Practitioners, demonstrate experience with value-based payment arrangements, and attest via questions to a limited set of advanced primary care delivery capabilities. Additional eligibility requirements (i.e., Medicare beneficiary volume) depends on if the practice is participating in either the PCF-general or the SIP-only or both payment model options. Additional details are available on the CMS website.
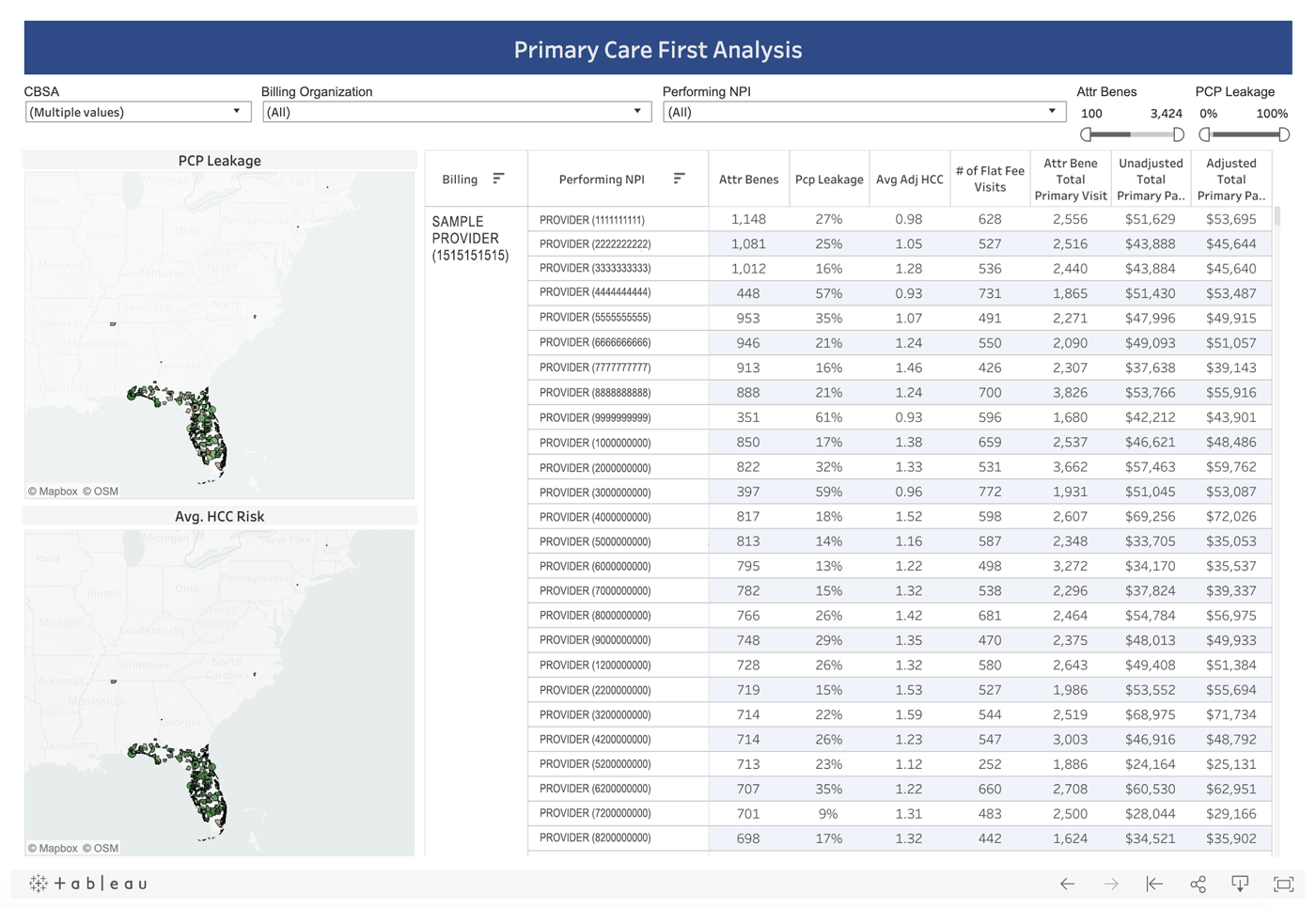
For the PCF-general payment model, the payments are composed of two types of payments, the Total Primary Care Payment (TPCP) and the Performance-Based Adjustment (PBA). The TPCP is composed of two subset of payments, the Professional Population-Based Payment and the Flat Primary Care Visit Fee. Leveraging our access to the full Medicare fee-for-service claims database, CareJourney has mapped claims data to the specifications in the PCF-general payment model. With the pending decision, organizations and primary care practices can use the CareJourney analysis to project their payment and determine whether PCF is appropriate for them.